Introduction: Facing a Denial From Your Health Insurer?
A health insurance attorney is a legal professional who helps policyholders fight claim denials, policy cancellations, and bad faith practices by insurance companies. You should consider hiring one when:
When to Hire a Health Insurance Attorney:
- Your claim for necessary treatment was denied – especially for serious conditions like cancer or heart disease
- You’ve exhausted internal appeals – and the insurance company still refuses to pay
- Your policy was unexpectedly cancelled – particularly after you filed a claim
- You suspect bad faith practices – such as deliberate delays, misrepresented policy terms, or refusal to investigate
- Your case involves ERISA plans – which have complex federal regulations and strict deadlines
- High-cost treatments are at stake – like proton beam therapy, residential mental health care, or experimental procedures
- You’re facing subrogation claims – where your insurer demands repayment from your settlement
Imagine being diagnosed with cancer and having your insurance company refuse to pay for your treatment. This nightmare scenario happens more often than you’d think. Health insurance companies deny millions of claims each year, and without legal counsel, the odds may not be in your favor when trying to fight a large corporation with teams of lawyers.
The reality is stark: You pay premiums every month expecting your insurer will be there when you need them most. But insurance companies often prioritize profits over patients, using complex policy language and aggressive tactics to avoid paying valid claims.
You don’t have to face this fight alone. A health insurance attorney understands the laws that protect you—like ERISA, the Affordable Care Act, and state bad faith statutes—and knows how to steer the appeals process, negotiate with insurers, and take your case to court if necessary.
Easy health insurance attorney glossary:
Why Health Insurance Companies Deny Claims
It’s a frustrating reality: you pay your premiums faithfully, expecting coverage when you need it most, only to be met with a “denied” stamp. Health insurance companies deny claims frequently, leading many policyholders to seek legal recourse. But why does this happen? Understanding the common reasons for denial can help us prepare for the fight ahead.

Here are some of the most common reasons we see claims denied:
- “Not Medically Necessary”: This is a big one. Insurance companies often use their own proprietary guidelines to define what is “medically necessary,” which can differ significantly from what your doctor believes is essential for your health. What one physician sees as vital, an insurer might deem “experimental” or “investigational.”
- “Experimental or Investigational Treatment”: New or cutting-edge treatments, even if recommended by specialists, might be labeled as experimental by your insurer to avoid coverage.
- Out-of-Network Provider: If you receive care from a doctor or facility not within your plan’s approved network, your claim might be denied or paid at a much lower rate.
- Failure to Obtain Pre-Authorization: Many plans require you to get approval from the insurance company before certain procedures, tests, or hospital stays. Forgetting this step, or having your doctor forget, can lead to a denial.
- Clerical Errors: Simple mistakes on paperwork—like an incorrect billing code, a misspelled name, or missing information—can cause a claim to be rejected. Sometimes it’s an honest oversight; other times, it feels like a convenient excuse.
- Policy Exclusions: Your health insurance policy is a contract, and it contains specific exclusions—services or conditions it won’t cover. These can be buried deep in the fine print.
- Untimeliness: Claims not submitted within the insurer’s specified timeframe can be denied.
- Pre-Existing Conditions: While the Affordable Care Act (ACA) largely eliminated denials based on pre-existing conditions, older “grandfathered plans” or certain short-term plans might still have limitations.
Understanding Bad Faith Insurance Practices
Beyond simple denials, sometimes insurance companies engage in what’s known as “bad faith” practices. This is when an insurer acts unreasonably or dishonestly in handling your claim, prioritizing their profits over their legal and ethical obligations to you, the policyholder. Bad faith practices by health insurers are illegal under federal law, and in some states, like Nevada, you have specific protections.
Common examples of bad faith include:
- Unreasonable Delays: Intentionally dragging their feet on investigating or paying a claim, causing you undue stress and financial hardship.
- Misrepresenting Policy Language: Deliberately misinterpreting the terms of your policy to deny or underpay a claim. They might claim a service isn’t covered when, by all reasonable interpretations, it should be.
- Failure to Investigate: Not conducting a proper investigation into your claim, or ignoring evidence that supports your need for coverage.
- Lowball Settlement Offers: Offering a significantly lower amount than what your claim is reasonably worth, pressuring you to accept less.
- Threatening the Policyholder: Using intimidation tactics or making veiled threats to discourage you from pursuing your claim.
- Cancelling Policies After Claims: This is particularly egregious. If an insurer cancels your policy after you’ve filed a large claim, alleging a minor error on your initial application, it could be a bad faith rescission.
When an insurer acts in bad faith, we may be able to pursue not only the benefits you’re owed but also additional damages, including punitive damages, to punish the insurer for their egregious conduct.
How Your Health Plan Type Affects Claims
The type of health insurance plan you have can significantly impact how your claims are handled and what challenges you might face.
- HMO (Health Maintenance Organization): These plans typically have lower premiums but restrict your coverage to a specific network of doctors and hospitals. You usually need a primary care physician (PCP) to refer you to specialists. Claims for out-of-network care are generally not covered, except in emergencies.
- PPO (Preferred Provider Organization): PPOs offer more flexibility, allowing you to see out-of-network doctors without a referral, though you’ll pay more. Claims for out-of-network care are covered, but at a higher cost to you.
- EPO (Exclusive Provider Organization): Similar to an HMO, EPOs require you to use doctors and hospitals within their network, but you don’t usually need a PCP referral to see a specialist. Like HMOs, out-of-network care is generally not covered.
Beyond these common structures, we also encounter:
- Self-Funded Employer Plans: Many large employers in Nevada and across the country offer self-funded plans. These are administered by an insurance company but the employer pays the claims directly. Crucially, these plans are often governed by a federal law called ERISA (Employee Retirement Income Security Act), which we’ll discuss more later. This means state laws, including bad faith laws, may not apply directly to them, adding a layer of complexity.
- Individual Plans: Obtained through the Affordable Care Act (ACA) marketplace or directly from insurers. These plans are subject to ACA protections, including coverage for essential health benefits and robust appeal rights.
- Grandfathered Plans: These are plans that existed on or before March 23, 2010, and haven’t undergone significant changes. They are exempt from some ACA requirements, including certain appeal rights. It’s important to know if your plan is grandfathered, as it affects your protections.
Understanding your plan type is the first step in understanding your rights and how to steer claim denials effectively.
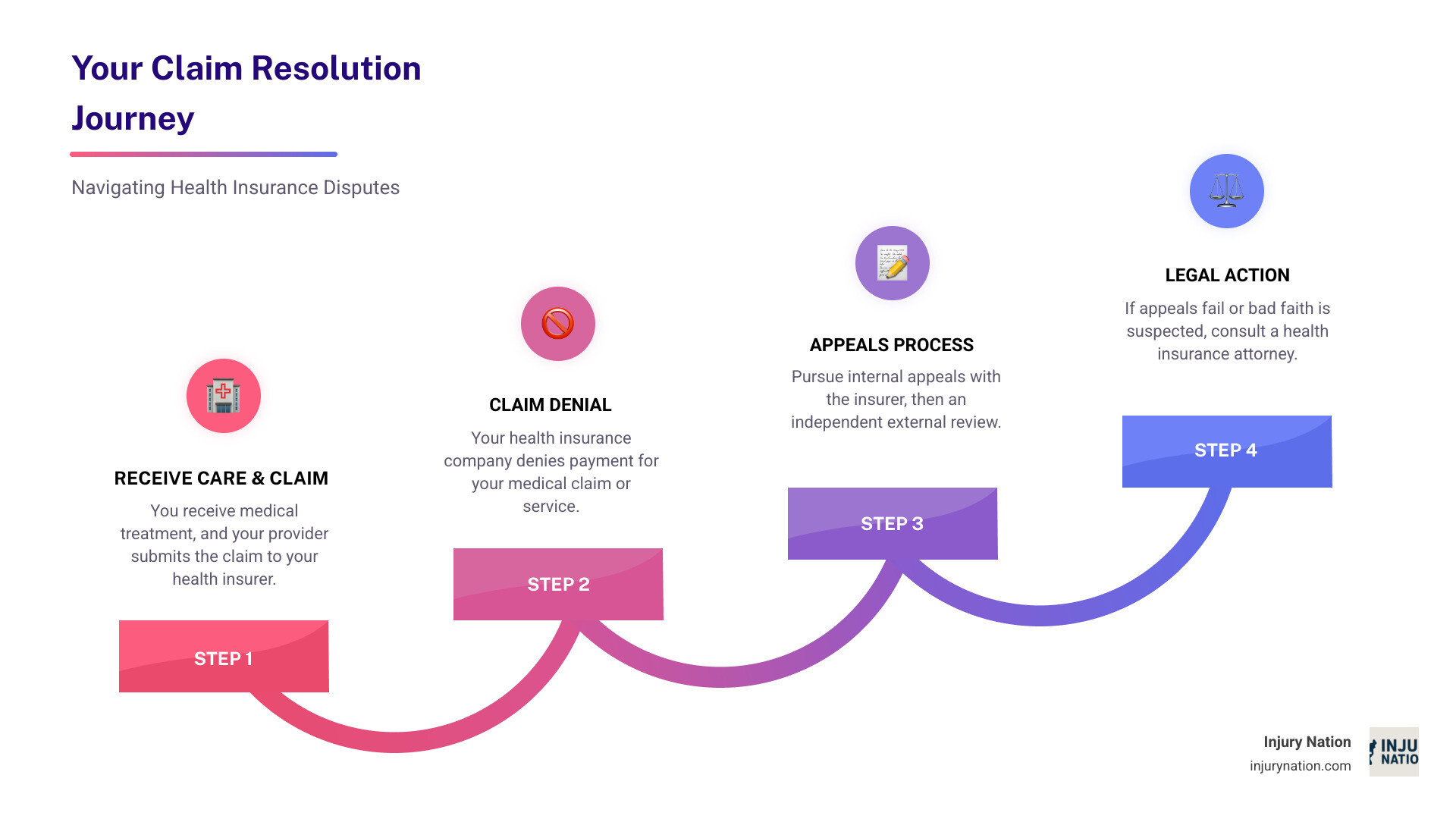
The Step-by-Step Process for Appealing a Denied Claim
Receiving a denied claim can feel like a punch to the gut, but it’s not the end of the road. We have rights, and there’s a clear process for appealing these decisions. The Affordable Care Act (ACA) ensures your right to appeal health insurance plan decisions, requiring your plan to reconsider its denial.

Here’s how we typically approach the appeals process:
Step 1: The Internal Appeal
Your first step is to appeal directly to your health insurance company. This is called an internal appeal, and it’s your right to ask your insurer to conduct a full and fair review of its decision.
- Review the Denial Letter Carefully: Your insurer must send you a letter explaining why your claim was denied, your right to an internal appeal, and your right to an external review if the internal appeal is unsuccessful. It should also mention the availability of a Consumer Assistance Program in your state.
- Gather Supporting Medical Evidence: This is crucial. Get a letter from your doctor explaining why the treatment or service was medically necessary. Include any relevant medical records, test results, and expert opinions that support your case.
- Follow Plan Procedures: Each insurer has specific forms and deadlines for internal appeals. Make sure you submit all required documentation within their timeframe. For urgent care, the decision must be made within 72 hours. For non-urgent care not yet received, it’s 30 days. For services already received, it’s 60 days.
- Keep Records: Document everything—dates of calls, names of people you spoke with, copies of all correspondence. This paper trail will be invaluable if you need to escalate your appeal.
We can help you steer this complex stage, ensuring all necessary documentation is submitted and your appeal is as strong as possible. For more information on your rights, visit Your right to appeal a health plan decision and The internal appeals process explained.
Step 2: The External Review
If your internal appeal is denied, don’t despair. You have the right to take your appeal to an independent third party for review. This is called an external review, and it means the insurance company no longer gets the final say over whether to pay a claim.
- Independent Review Organization (IRO): An IRO is an independent entity that reviews your medical information and your insurer’s decision. Their decision is usually binding on your health plan.
- Timelines: You typically have 60 days from receiving your internal appeal denial to request an external review.
- State Resources: Your state may have a Consumer Assistance Program that can help you file an appeal or request a review. In Nevada, you can contact your state insurance regulator for guidance on external reviews.
An experienced health insurance attorney can be instrumental during this stage, presenting your case to the IRO in the most compelling way possible. To understand more about this process, see How external reviews work. You can also contact your state insurance regulator for specific guidance in Nevada.
When and How to Hire a Health Insurance Attorney
While the appeals process is designed for policyholders, it can be incredibly complex and intimidating, especially when you’re dealing with a serious health issue. This is where a health insurance attorney becomes your indispensable advocate.
You might be asking yourself, “When should we bring in legal counsel?” We recommend considering it if:
- Your case is complex or involves high-cost treatments: If you’re fighting for coverage of expensive procedures like proton beam radiation therapy, residential mental health treatment, or gender-affirming care, the stakes are high, and the insurer’s resistance might be formidable.
- You suspect bad faith practices: As we discussed, if you believe your insurer is intentionally delaying, misrepresenting, or unfairly denying your claim, a lawyer can help investigate and pursue a bad faith claim.
- You’ve exhausted internal and external appeals: If you’ve been through the entire appeals process and still haven’t received coverage, your next step might be litigation, which absolutely requires legal expertise.
- Your policy is tied to an employer (ERISA plan): These plans fall under federal law, which has its own intricate rules and deadlines. A lawyer specializing in ERISA claims is crucial here.
- You’re facing a subrogation claim: If your health insurer is demanding repayment from a personal injury settlement, an attorney can help negotiate these claims, potentially increasing the amount you keep.
The benefits of legal guidance are clear: we level the playing field against powerful insurance companies, protecting your rights and fighting for the coverage you deserve.
What Does a Health Insurance Attorney Do?
A health insurance attorney is a specialized legal professional dedicated to helping you steer the often-turbulent waters of health insurance disputes. Here’s a glimpse into what we do:
- Case Evaluation: We’ll review your policy, denial letters, medical records, and all communications to assess the strength of your case and outline your legal options.
- Evidence Gathering: We help you collect crucial medical documentation, expert opinions, and other evidence to bolster your claim.
- Communicating with Insurer: We handle all correspondence and negotiations with the insurance company, speaking their language and ensuring your rights are protected.
- Navigating ERISA: If your plan is employer-provided, we understand the nuances of ERISA law, which dictates strict deadlines and administrative procedures that must be followed.
- Negotiating Settlements: Our goal is often to negotiate a fair settlement that gets your medical bills covered and, in cases of bad faith, secures additional compensation.
- Filing Lawsuits: If negotiations fail or bad faith is evident, we are prepared to take your case to court, advocating for you before a judge and jury.
- Protecting Your Rights: Our role is to ensure your insurer upholds its end of the contract and that you receive the health benefits you’ve paid for.
How to Choose the Right Health Insurance Attorney
Choosing the right health insurance attorney in Nevada is a critical decision. Here’s what we recommend looking for:
- Experience with Health Insurance Law: This is a specialized field. Look for attorneys with a proven track record in handling health insurance disputes, not just general personal injury or insurance law.
- Track Record of Success: Ask about their past cases, especially those similar to yours. While past results don’t guarantee future outcomes, they indicate competence.
- Communication Skills: You need an attorney who can clearly explain complex legal concepts and keep you informed every step of the way. You should feel comfortable asking questions and receiving straightforward answers.
- Fee Structures: Understand how they charge for their services. Many work on a contingency fee basis for denied claims, meaning we only get paid if you win.
- Client Testimonials: Reviews and testimonials can offer insights into an attorney’s professionalism, empathy, and effectiveness.
- Personalized Attention: You want an attorney who will treat your case with the individual attention it deserves, not just as another file.
Preparing for Your Consultation
Coming prepared to your initial consultation with a health insurance attorney can make a huge difference. It helps us quickly understand your situation and advise you effectively.
Here’s a list of documents and information we’ll typically want to review:
- Your Health Insurance Policy: Bring a complete copy of your policy, including all riders, amendments, and the Summary Plan Description.
- All Denial Letters: Every letter you’ve received from your insurance company regarding the denied claim, including explanations of benefits (EOBs).
- All Correspondence: Any emails, letters, or written communications between you, your medical providers, and the insurance company.
- Medical Records and Bills: All relevant medical records related to the denied claim, including doctor’s notes, test results, diagnoses, and itemized medical bills.
- Timeline of Events: A chronological summary of what happened, from when you sought treatment to when you received the denial, including dates of calls and who you spoke with.
- List of Questions: Don’t be shy! Write down all your questions and concerns so we can address them during our meeting.
The more information you provide, the better we can assess your case and determine the best course of action.
Key Laws That Protect Your Health Insurance Rights
Fortunately, you’re not entirely at the mercy of insurance companies. A complex web of federal and state laws exists to protect policyholders and ensure fair treatment. A knowledgeable health insurance attorney understands these laws and how to use them to your advantage.
ERISA (Employee Retirement Income Security Act)
If your health insurance plan is provided by your employer (and is not a government or church plan), it’s highly likely governed by the Employee Retirement Income Security Act of 1974, or ERISA. This federal law sets minimum standards for most voluntarily established retirement and health plans in private industry.
- Federal Preemption: One of the most significant aspects of ERISA is that it often “preempts” state laws. This means that if your claim is denied under an ERISA plan, state bad faith laws, which often allow for greater damages, may not apply.
- Strict Deadlines: ERISA outlines specific, often strict, deadlines for appealing denied claims, both internally and externally. Missing these deadlines can jeopardize your entire case.
- Administrative Record: Under ERISA, any lawsuit challenging a denial is generally limited to the “administrative record”—the documents and information submitted to the plan during the internal appeals process. This makes the internal appeal stage incredibly important for ERISA claims.
- How it Impacts Lawsuits: Successfully litigating an ERISA case requires deep knowledge of its procedural requirements and judicial interpretations. An ERISA health insurance attorney is essential to steer these complexities and build a strong case.
ACA and MHPAEA Protections
Two other crucial pieces of legislation provide significant protections:
- Affordable Care Act (ACA): The ACA, passed in 2010, brought widespread reforms to the health insurance market. It requires most plans (those not “grandfathered”) to cover essential health benefits, eliminated annual and lifetime limits on coverage for essential health benefits, and ensures you can’t be denied coverage due to pre-existing conditions. Crucially, it also strengthened your right to internal and external appeals for denied claims and prevents insurance companies from canceling your coverage just because you or your employer made an honest mistake on your application. They must notify you at least 30 days before canceling coverage, and only for specific reasons like intentional false information or non-payment of premiums.
- Mental Health Parity and Addiction Equity Act (MHPAEA): This act, often referred to as the “Mental Health Parity Law,” requires most health plans that offer mental health and substance use disorder benefits to provide them in a way that is no more restrictive than medical and surgical benefits. This means things like co-pays, deductibles, out-of-pocket maximums, and treatment limits for mental health care must be comparable to those for physical health care. If your mental health or substance use disorder claim is denied because the insurer treats it differently than a physical health claim, an attorney can help you fight for parity.
These laws, alongside state-specific regulations in Nevada, form the legal framework that a health insurance attorney uses to protect your rights and challenge unfair denials.
Frequently Asked Questions about Health Insurance Lawyers
We often hear similar questions from individuals struggling with health insurance issues. Let’s address some of the most common ones.
What are the costs of hiring a health insurance attorney?
The cost of hiring a health insurance attorney can vary significantly based on several factors, including the complexity of your case, the attorney’s experience, and the firm’s size. However, we understand that medical bills are already a burden, so many firms, including those we work with, offer flexible fee arrangements:
- Contingency Fees: This is very common, especially for denied claims where a financial recovery is sought. With a contingency fee, the lawyer only gets paid if they recover money for you, typically a percentage (between 20% and 50%) of the recovered amount. This means no upfront costs or out-of-pocket expenses for you.
- Hourly Rates: Some attorneys charge an hourly rate, which can range from $100 to $1,000, depending on the factors mentioned above. This is more common for advisory roles or less complex disputes.
- Retainer Fees: An upfront payment that covers a certain amount of work.
- Free Consultations: Many reputable health insurance attorneys offer free initial consultations. This allows you to discuss your case without financial commitment and determine if legal action is viable.
Our goal at Injury Nation is to connect you with attorneys who operate on a “no win, no fee” promise, ensuring that financial concerns don’t prevent you from seeking justice.
Can I sue my health insurance company?
Yes, you absolutely can sue your health insurance company, but it’s usually a last resort after exhausting the appeals process.
- Grounds for a Lawsuit: You might have grounds to sue if your claim was wrongfully denied, if the insurer acted in bad faith, or if they breached their contract with you (your policy).
- After the Appeals Process: For most plans, you must go through the internal and external appeals process before you can file a lawsuit. This is especially true for ERISA plans.
- Bad Faith Claims: If we can prove your insurer engaged in bad faith practices—like intentionally delaying payments or misrepresenting policy terms—we may be able to seek not only the benefits you’re owed but also additional damages, including punitive damages, to punish the insurer for their misconduct.
- Breach of Contract: Your health insurance policy is a contract. If the insurer fails to uphold their end of the agreement by denying a valid claim, they have breached that contract.
- Potential Damages: A successful lawsuit could recover the cost of your medical treatment, interest on the unpaid amount, damages for emotional distress, and in bad faith cases, punitive damages.
Suing a large insurance company is a complex undertaking, requiring significant legal expertise. That’s why having an experienced health insurance attorney by your side is crucial.
How long does a health insurance dispute take to resolve?
The timeline for resolving a health insurance dispute can vary greatly, depending on several factors:
- Case Complexity: Simple clerical errors might be resolved quickly through a phone call or a single internal appeal. Complex cases involving experimental treatments or large sums of money will naturally take longer.
- Appeal Timelines: As discussed, internal appeals have deadlines (72 hours for urgent care, up to 60 days for services already received). External reviews also have their own timelines.
- Negotiation Period: If we enter into negotiations with the insurer, this can take weeks or months, depending on their willingness to settle.
- Litigation Timeline: If a lawsuit becomes necessary, the process can be lengthy. Court cases can take anywhere from several months to several years, depending on the court’s schedule, findy, and whether the case goes to trial.
While we always strive for the quickest resolution possible, our priority is to achieve the best outcome for you, even if it takes time. We will keep you informed every step of the way.
Find the Right Advocate to Fight for Your Health
Navigating the labyrinthine world of health insurance denials can feel like an impossible task, especially when you’re already facing health challenges. But as we’ve explored, you have significant legal rights as a policyholder, and you don’t have to face powerful insurance companies alone.
The value of legal representation cannot be overstated. A skilled health insurance attorney can decipher complex policy language, challenge wrongful denials, identify bad faith practices, and guide you through the intricate appeals process, all while fighting to ensure you receive the coverage you deserve. Whether it’s a denied claim for life-saving treatment, an unfair policy cancellation, or a subrogation demand eating into your personal injury settlement, an attorney is your advocate.
Don’t let insurance giants intimidate you into accepting less than you’re entitled to. If your health insurance claim has been denied, or you’re struggling with any health insurance dispute in Nevada, it’s time to seek expert legal guidance.
We’re here to help you find the right advocate. Visit our directory to Find a personal injury lawyer to help with your insurance dispute and connect with a top-rated health insurance attorney who can fight for your health and your rights.



